Telemedicine is Changing How Long-Term Care Facilities are Managed
DigiGone • September 8, 2020
Telemedicine is emerging as a sustainable solution for residents at long-term facilities. Not only is it safer for both patients and care providers, but it also enhances treatment options, and it’s financially sustainable.

Patients in long-term care facilities are some of the most vulnerable members of our communities. Chronic diseases, comorbidities and strenuous rehabilitation regimes make their care both critical and complicated. Layered on top of that is the fatal risk of exposure to COVID-19; as of Sept. 7, 2020, more than 50,000 patients
in long-term care (LTC) facilities had died from the COVID-19 virus, which accounts for more than 40% of all US deaths.
Improved Collaboration for Better Care
Karen S. Rheuban MD, director and co-founder of the University of Virginia Center for Telehealth, spoke
with the American Medical Association (AMA) recently and explained that since the arrival of COVID-19, they’ve had to transition their focus and compared this shift to a Blockbuster versus Netflix model: Instead of using telehealth services to increase access to just primary care and urgent care during normal business hours, it has taken on a much broader scope. Care is drastically improved through remote collaboration with dialysis centers, clinics and other specialty provider locations, 24/7. This applies to both inpatient and outpatient use.
Real Case Scenario
In August, Dr. Laurie Archbald-Pannone, a geriatric specialist and associate professor of medicine at the University of Virginia, shared their approach in developing a collaborative care model using telemedicine.
Together with doctors, nurses, emergency responders and local public health experts, they studied how hospitals and academic medical centers can work successfully with LTC facilities.
In addition to coordinating widespread testing, Dr. Archbald-Pannone explains, “We have improved their [patient] access to sub-specialty care with telemedicine, a great tool for patients.”
To establish these collaborative virtual appointments, a nurse practitioner leads a telementoring training program for facility administrators and clinical teams, addressing any technical questions prior to the first appointment.
“We helped arrange telemedicine visits with critical care doctors who used a virtual stethoscope to listen to heart and lung sounds remotely and connect in a real-time video chat with a resident, nurse and primary care physician. This kind of care, we discovered, is effective, efficient and much easier on the resident; instead of a trip to the hospital or doctor’s office, patients can receive treatment and talk to a physician from the nursing home.”
Dr. Archbald-Pannone points out that telemedicine also helps to alleviate chronic staffing problems at LTCs. With greater access to doctors and timely treatment, patients recover quicker and require fewer transfers to larger facilities, again, reducing their risk of exposure.
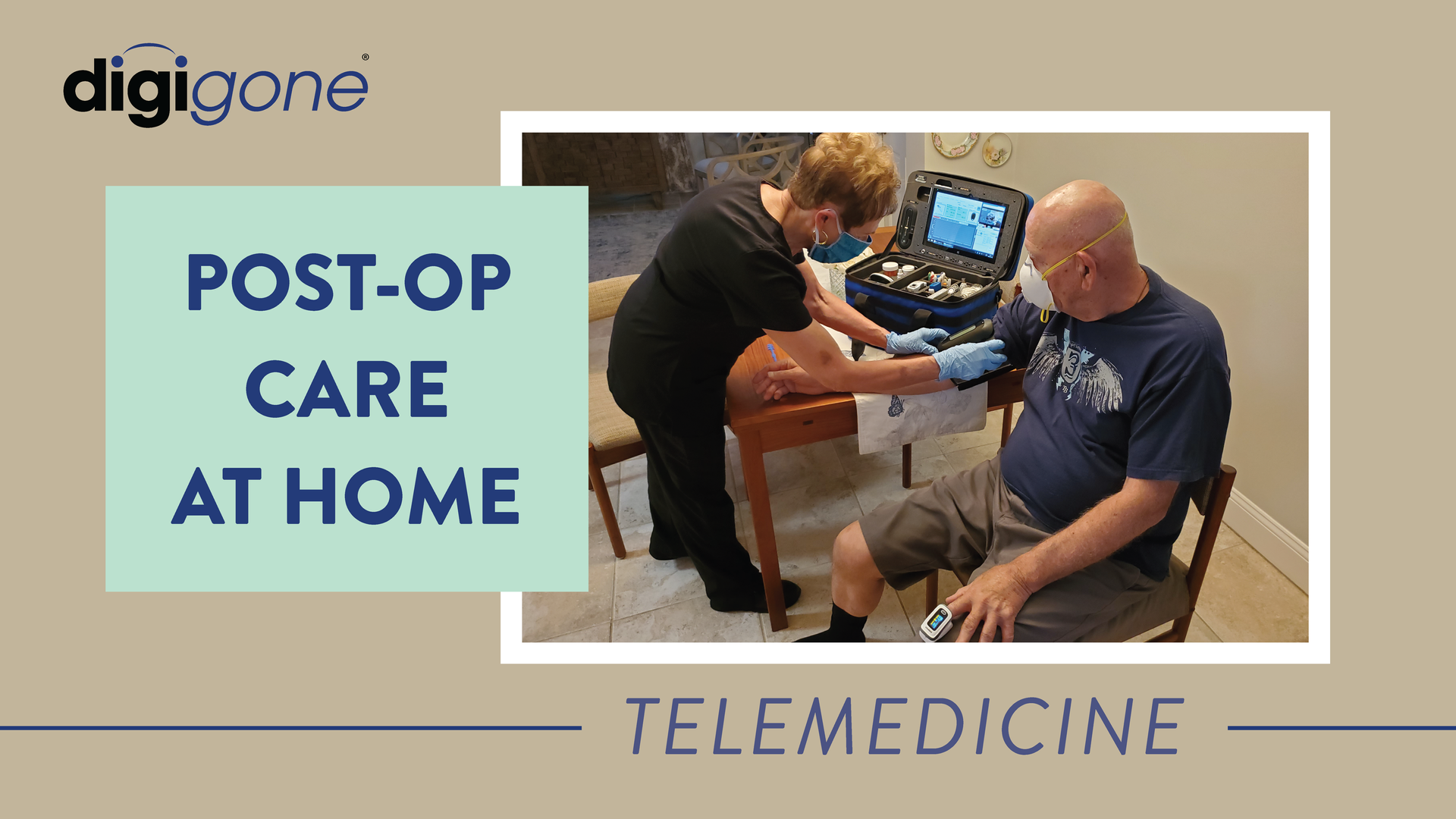
Comprehensive Diagnostic Tools
Telemedicine kits allow for real-time virtual consultations through an encrypted video-conferencing application, providing a continuum of care in a safe environment. Diagnostic data shared through HIPPA-compliant software allows specialists to make immediate care decisions.
Other tools available in telemedicine kits include an electrocardiogram, electronic stethoscope, otoscope and an ultrasound device, all of which can be remotely controlled by specialists. A telemedicine kit can easily be carried to a patient’s room, or set up as a virtual walk-in clinic anywhere.
The telemedicine kit needs to be easy to use, training should be simple and hands-on. In addition, the kit needs to be affordable and integrate with existing Internet connectivity and able to export patient data into existing medical record systems.
The Bottom Line
On the Aug. 10 episode of the AMA’s virtual daily update, medical leaders and experts tackled the very complicated issue of the cost associated with virtual innovation in treating patients.
Nick Doughtery, managing director at Mass Challenge Health Tech, participated in the call and, after talking about telemedicine, offered the following:
“They [care providers] think so much about the patient, but they forget that this lives within a world where you have to be able to afford it, or it has to be able to create that return on investment. Otherwise, it's not going to be adopted.”
Vice president of managed accounts at Moving Analytics
Beth Andrews, illustrated the ROI succinctly:
“When you look at the area that we're in, in providing virtual cardiac rehab, currently patients are participating at under 20%. Our [virtual] programs are achieving over 80% participation.
“And when you complete cardiac rehab, you are doubling your post-event life expectancy. You are reducing your chances of a second event. And you are also able to increase your health factors. Health systems and health plans, insurers, they are seeing a reduction in readmissions. So it all just makes sense. And we see that acceleration now, and it's here to stay.
“When we start seeing patients recovering quicker, requiring less transfers, the bottom line for their health and overall medical costs are positively impacted.”
Compound Value
When compounding the value of collaborative managed care available 24/7 in a low-risk environment, while at the same creating faster recovery times and more positive health outcomes and creating a positive ROI, it’s a resounding win-win.

Telemedicine kits are becoming indispensable tools for home healthcare providers, particularly during transition care medical examinations (TCMs). While the initial TCM is conducted by a physician who generates revenue from the service, the telemedicine kit significantly benefits home healthcare providers by expediting patient registration for their care services. With a nurse or medical assistant deploying the kit, patients can be quickly evaluated and connected with a physician, ensuring all necessary documentation and approvals are completed more efficiently. This faster onboarding process allows home healthcare providers to register more patients in less time, helping them deliver care sooner and grow their services efficiently. The ability to “bring the doctor” to the patient through a telemedicine kit is invaluable in initiating care seamlessly. Once patients are on board, home healthcare providers can continue leveraging telemedicine technology to improve how they deliver services. The kits enable nurses and medical assistants to perform follow-up visits, diagnostics, and real-time consultations without requiring patients to leave their homes. This capability allows providers to optimize their schedules and visit more patients daily, all while maintaining a high standard of care. The efficiency gained means better coverage, smarter use of resources, and happier patients. Beyond efficiency, telemedicine kits help providers build stronger connections with their patients by making care more accessible and personalized. Providers can quickly respond to emerging health concerns, adjust care plans, and ensure ongoing monitoring—all from the patient’s home. This not only leads to better patient outcomes but also boosts the provider’s reputation for being reliable and innovative. By facilitating the registration of more patients and enhancing care once they are onboarded, telemedicine kits are powerful tools that enable home healthcare providers to expand their reach, improve operational efficiency, and thrive in an increasingly competitive market. In a rapidly evolving healthcare landscape, telemedicine kits are revolutionizing how home healthcare providers deliver care, enabling faster patient onboarding, enhanced service delivery, and stronger connections with patients. By integrating this indispensable technology, providers can streamline operations, improve patient outcomes, and position themselves as leaders in care innovation. Don’t miss the opportunity to elevate your home healthcare services. Explore how telemedicine kits can help you expand your reach, optimize your resources, and deliver exceptional care. Contact us today to learn more and take the next step toward transforming your care delivery model.

With the new Safer Seas Act, vessel companies must comply with many new regulations by the end of the year. One of those requirements includes audio equipment placed outside of hallways leading to staterooms, which DigiGone can help with. And while this may seem burdensome, these new rules will be good for vessel companies in the long run.