Five Reasons Why Telemedicine is the Right Cure at Just the Right Time
DigiGone • June 29, 2020

The future of telemedicine
is bright. Patients across the country are getting their first dose of virtual care and, for the most part, they love it. Many see crowded waiting rooms a thing of the past, as perhaps they should be.
The telemedicine industry as a whole was thrust into the spotlight when the pandemic hit, but fortunately the major components and technologies were already in place allowing for an almost seamless move to virtual care.
Here’s a look at five key factors that contributed to the success of telemedicine, all of which will sustain it long term.
Remote Monitoring for Ongoing Care
One of the most important aspects of telemedicine
is that it allows high-risk patients who require ongoing care to stay isolated as much as possible. Of course, diagnosis, treatment plans and consultations will often be handled in-person. But after, say, an arduous chemotherapy regimen or surgery, instead of asking a patient to travel to a crowded hospital, remote health care allows them to stay home, greatly reducing the risk of contracting an infection or virus.
Medical facilities are investing millions into infrastructure to support this type of remote care. Just recently, Baystate Medical Center in Springfield, MA, was granted almost $1 million through the CARES Act to procure “remote monitoring platforms focused on obstetrics, diabetes, and hypertension, (...) and videoconferencing equipment to enable telehealth visits.”
As well, Stony Brook University Hospital of New York was awarded just under $1 million for similar platforms to “enhance virtual visits” for on-going care for high-risk patients.
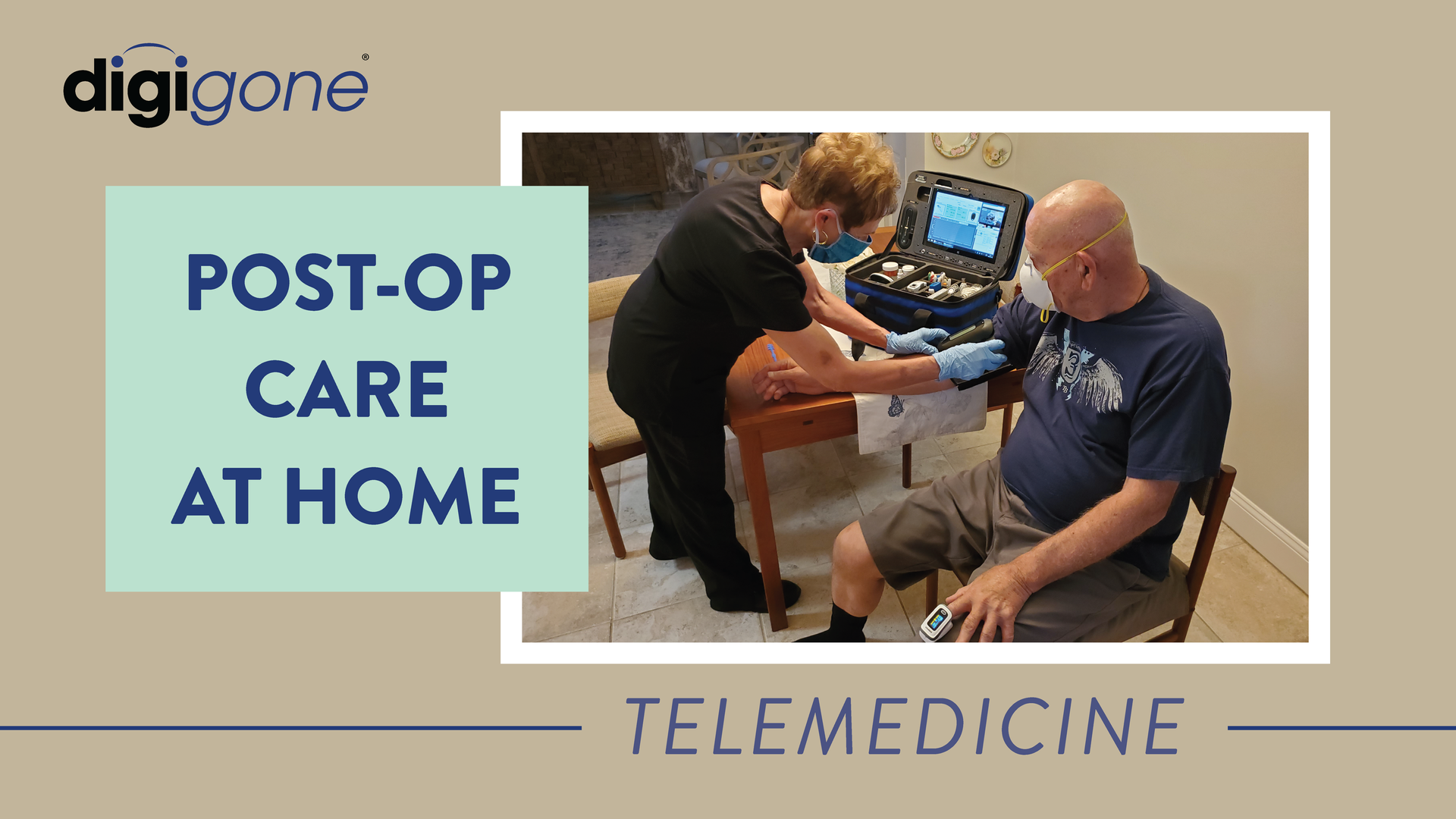
With a telemedicine kit, patients can check-in virtually, upload basic diagnostic information and speak to a doctor. The technology and tools are simple to use and can be controlled remotely by the medical provider.
In other scenarios, a nurse can travel to the homes of patients to gather basic diagnostic information, just like they would at an office, then share scans, screens and data from the telemedicine kit with a doctor.
Faster Internet For All
Broadband internet infrastructure has long been a major obstacle in enhanced remote health care. But, now the government is stepping in. Legislators have recently introduced bills aimed at channeling funds to rural areas; like the Moving Forward Act
which would direct $1.5 trillion toward rebuilding broadband internet infrastructure in underserved communities, “prioritizing those with persistent poverty.”
Another bill
that was recently introduced is strictly aimed at speeding up the process. The Accelerating Broadband Connectivity Act incentivizes “winning bidders of the Rural Digital Opportunity Fund auction to complete their build-out obligations on a shorter timeline.”
Triage Care Anywhere
In terms of triage care at remote locations, telemedicine kits
pack a powerful punch. Many come equipped with all the basic tools found in a doctor’s office, such as a pulse oximeter, glucose meter, digital thermometer, electrocardiogram, stethoscope, otoscope and optional equipment, like ultrasound tools. This means that a walk-in clinic can be set-up anywhere. Instead of ambulatory services, health care providers can deploy teams of medical assistants to areas and with a telemedicine kit
provide the same services patients would receive at a hospital.
This type of coordinated large-scale care is often rolled out after natural disasters; instead of patients traveling to a hospital, which might be impossible for a multitude of reasons, groups of medics travel to patients. Two key features of telemedicine kits
make this possible: a satellite terminal ensuring reliable connectivity and a solar power kit which ensures the kits stay charged all the time.
Care can then be monitored and coordinated at one location, while doctors remotely triage and diagnose patients in the field.
Portable Ultrasound Tools
The advancement of portable ultrasound tools has been a game changer in fighting the COVID-19 pandemic. In Africa and Europe, doctors have used the devices to examine lung health of patients battling the novel coronavirus. Using this small pocket-sized tool, they can assess the severity of infection and then determine the level of care required.
Also, physicians in the field are able share their screen (or scans) with specialists in real-time at a central location. This allows for a greater coordination of care and for more patients to be screened and treated.
Secured Connections, Advanced Technology
A big concern with the adoption of telemedicine was liability. Recently the publication Insurance Business spoke with Greg Ferrell, vice president of professional liability for Admire Insurance Group, about patient safety and privacy.
“I don’t think it can be sold high enough that the relief this activity [telemedicine] gives to hospitals and urgent clinics is massive,” Ferrell said. “If everyone who was using a telemedicine platform to see a provider right now was standing in line at the hospital, the healthcare system would be completely overwhelmed.”
With that, Ferrell said we’re fortunate that the pandemic happened now and not five years ago, when there would have been significant security concerns.
“In a way the emergence of COVID-19 and the practice of telemedicine to address it came at a good time in that telemedicine has been ramping up so much over the last few years that the technology is really pretty spot on, and so is the security,” Ferrel said.
Putting all of these factors together – remote care capabilities, far-reaching broadband connectivity, mobile and triage units, sophisticated equipment and heightened security – the importance of telemedicine
during the pandemic is simply invaluable.
And now that a large swatch of patients and doctors have realized its full benefits and potential, luckily, it’s here to stay.

Telemedicine kits are becoming indispensable tools for home healthcare providers, particularly during transition care medical examinations (TCMs). While the initial TCM is conducted by a physician who generates revenue from the service, the telemedicine kit significantly benefits home healthcare providers by expediting patient registration for their care services. With a nurse or medical assistant deploying the kit, patients can be quickly evaluated and connected with a physician, ensuring all necessary documentation and approvals are completed more efficiently. This faster onboarding process allows home healthcare providers to register more patients in less time, helping them deliver care sooner and grow their services efficiently. The ability to “bring the doctor” to the patient through a telemedicine kit is invaluable in initiating care seamlessly. Once patients are on board, home healthcare providers can continue leveraging telemedicine technology to improve how they deliver services. The kits enable nurses and medical assistants to perform follow-up visits, diagnostics, and real-time consultations without requiring patients to leave their homes. This capability allows providers to optimize their schedules and visit more patients daily, all while maintaining a high standard of care. The efficiency gained means better coverage, smarter use of resources, and happier patients. Beyond efficiency, telemedicine kits help providers build stronger connections with their patients by making care more accessible and personalized. Providers can quickly respond to emerging health concerns, adjust care plans, and ensure ongoing monitoring—all from the patient’s home. This not only leads to better patient outcomes but also boosts the provider’s reputation for being reliable and innovative. By facilitating the registration of more patients and enhancing care once they are onboarded, telemedicine kits are powerful tools that enable home healthcare providers to expand their reach, improve operational efficiency, and thrive in an increasingly competitive market. In a rapidly evolving healthcare landscape, telemedicine kits are revolutionizing how home healthcare providers deliver care, enabling faster patient onboarding, enhanced service delivery, and stronger connections with patients. By integrating this indispensable technology, providers can streamline operations, improve patient outcomes, and position themselves as leaders in care innovation. Don’t miss the opportunity to elevate your home healthcare services. Explore how telemedicine kits can help you expand your reach, optimize your resources, and deliver exceptional care. Contact us today to learn more and take the next step toward transforming your care delivery model.

With the new Safer Seas Act, vessel companies must comply with many new regulations by the end of the year. One of those requirements includes audio equipment placed outside of hallways leading to staterooms, which DigiGone can help with. And while this may seem burdensome, these new rules will be good for vessel companies in the long run.